- PATHOLOGY / SYMPTOMS:
- Benign prostatic hyperplasia
- Pyeloureteral junction syndrome
- Ureteral stricture
- Urethral stricture
- Laser in Urology
- TREATMENTS:
- BENIGN PROSTATIC HYPERPLASIA.
- PYELOURETERAL JUNCTION SYNDROME.
- URETERAL STENOSIS.
- URETRAL STENOSIS.
- LASER IN UROLOGY.
Benign prostatic hyperplasia
The prostate is an organ located in the male pelvis, just below the bladder, hugging the urethra. Its function is basically sexual, participating in the formation of seminal fluid and contraction at the time of ejaculation.
Benign prostatic hyperplasia is the result of noncancerous growth of the tissue that makes up the prostate. Its causes are not known, but it seems to be related to hormonal changes that occur with aging. By the age of 60, half of the male population already has microscopic signs of benign prostatic hypertrophy (BPH) and by the age of 70, more than 40% have an increase in prostate size that can be detected with scanning. The normal size of the prostate is similar to that of a chestnut.
Symptoms
In people with an enlarged prostate, the severity of symptoms varies, but they tend to gradually worsen over time. Common signs and symptoms of benign prostatic hyperplasia include:
- Need to urinate frequently or urgently
- Increased frequency of urine at night (nocturia)
- Difficulty starting to urinate
- Weak or stopping and restarting urine flow
- Drip after urinating
- Inability to empty the bladder completely
Less common signs and symptoms include:
- Urinary tract infection
- Inability to urinate
- Blood in the urine
The size of the prostate does not necessarily determine the severity of symptoms. Some men with a mildly enlarged prostate may have significant symptoms while other men with a larger prostate may have only mild symptoms.
Differential diagnosis
Diseases that produce symptoms similar to those of an enlarged prostate include:
- Urinary tract infection
- Inflammation of the prostate (prostatitis)
- Narrowing of the urethra (urethral stenosis)
- Scarring of the bladder neck as a result of previous surgeries
- Kidney or bladder stones
- Problems with the nerves that control the bladder
- Prostate or bladder cancer
Aetiology
The prostate gland is located below the bladder. The tube that carries urine from the bladder to the outside of the penis (urethra) passes through the center of the prostate. When the prostate enlarges, it begins to obstruct the flow of urine.
Most men have continuous prostate growth throughout life. In many men, this continuous growth enlarges the prostate enough to cause urinary symptoms or to significantly obstruct the flow of urine.
It’s not entirely clear what causes an enlarged prostate. However, it could be due to changes in the balance of sex hormones as men age.
Risk factors
Risk factors for enlarged prostate glands include the following:
- Aging. Enlarged prostate glands rarely cause signs and symptoms in men younger than 40. About one-third of men experience moderate to severe symptoms by age 60, and about half by age 80.
- Family history. Having an affected blood relative, such as a parent or sibling, means you’re more likely to have problems.
- Lifestyle. Obesity increases the risk of benign prostatic hyperplasia, while exercise can reduce it.
Complications
Complications of an enlarged prostate may include:
- Sudden inability to urinate (urinary retention)). You may need to have a tube (tube) inserted into your bladder to drain urine. Some men with an enlarged prostate require surgery to relieve urinary retention.
- Urinary tract infections. The inability to completely empty the bladder can increase the risk of urinary tract infection. If urinary tract infections occur frequently, you may need surgery to remove part of your prostate.
- Bladder stones. Bladder stones occur due to the inability to completely empty the bladder. Bladder stones can cause infection, bladder irritation, blood in the urine, and obstruction of urine flow.
- Bladder damage. If the bladder has not completely emptied, this can cause it to stretch and weaken over time. As a consequence, the muscular wall of the bladder no longer contracts properly and this makes it more difficult to completely empty the bladder.
- Kidney damage. Pressure on the bladder due to urinary retention can directly damage the kidneys or allow bladder infections to reach the kidneys.
Most men with an enlarged prostate do not develop these complications. However, acute urinary retention and damage to the kidneys can pose serious health hazards.
Diagnosis
Medical history it is essential for diagnosing BPH and the severity of lower urinary tract symptoms. In our practice, the urologist may use resources such as Quality of life questionnaires to numerically assess the degree to which the pathology affects the patient.
Physical exam, including digital rectal examination, is fundamental. By means of digital rectal examination, the morphology and consistency of the prostate is assessed and at the same time the tone of the anal sphincter is evaluated.
Some complementary examinations are also very useful, and include a urinalysis (by dipstick or culture) to rule out a possible urinary tract infection, the determination of PSA, the assessment of renal function and an ultrasound study (transrectal and/or abdominal). Performing a renewal-resonography will rule out possible complications (urinary lithiasis, bladder diverticula, dilatation of the urinary tract, renal or bladder tumors) and quantify the post-voiding residue. It is a simple method that has no contraindications or risks and that allows estimating the volume and prostatic morphology quite accurately.
In addition, in most cases a flowmetry is carried out, which is a simple study that objectively measures the flow of the urinary stream, and allows us to classify the flow into obstructive or non-obstructive.
Other more complex tests, such as the urodynamic study, will be performed in specific cases, in which the prostate symptomatology is associated with other pathologies (neurological, intrinsic bladder) or when the diagnosis is not so clear with conventional tests.
Currently, European clinical guidelines in Urology recommend the annual performance of PSA and the practice of digital rectal examination in men over 50 years of age as methods of screening for prostate cancer and monitoring of BPH. Some authors consider that in people under 50 years of age it is only advisable to screen individuals at high risk of presenting it due to the existence of a family history of cancer. In this case, they start the study from the age of 40.
In our facilities of Uros Associats we can perform all the complementary examinations commented: Ultrasound, flowmetry and urodynamic study,
Treatment
Treatment of benign prostatic hyperplasia can vary, depending on the severity of symptoms and how they affect the patient’s quality of life.
Adrenergic blocking drugs They can help patients with mild and moderate symptoms. They are medicines that are taken once a day, every day. Its function is based on decreasing resistance to urinary flow without modifying the contractility of the bladder muscle. They relax the muscle tone of the bladder neck and prostate, improving symptoms and maximum urinary flow. They are not exempt from side effects: retrograde ejaculation, headaches, asthenia, drowsiness, nausea, nasal congestion, dizzying sensation and dizziness due to orthostatic hypotension (sudden decrease in blood pressure), which constitutes the worst tolerated secondaryism, although it may disappear over weeks, as the body makes compensatory internal adjustments in blood pressure.
Hormone-blocking drugs They induce a regression of the increase in prostate size and increase the speed of maximum urinary flow, thus improving the patient’s symptoms. They have the disadvantage that they take time to be effective (minimum 6 months) and that they can occasionally cause disorders of sexual function (decreased libido, ejaculatory dysfunction and impotence) and others such as gynecomastia, increased breast sensitivity and skin rashes. These drugs also lower serum PSA to 50%.
Phytotherapy It consists of the application of plant extracts (Pygeum africanum, Serenoa repens), whose mechanism of action is not clearly known. They produce variable urodynamic improvements. They have few side effects and their economic cost is low.
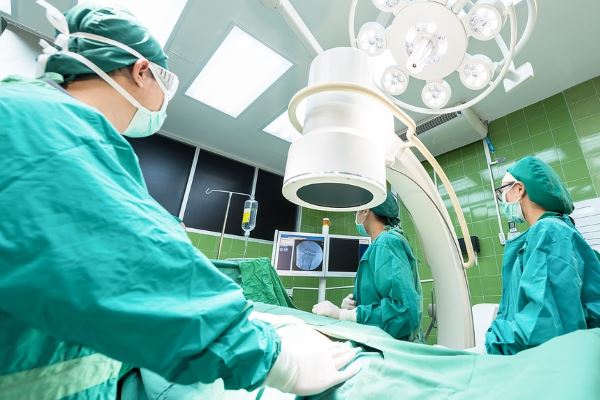
Surgery is the most effective treatment for BPH. It has several modalities: endourological surgery, which is performed through the urethral duct, without skin incisions (transurethral resection or P-TUR, prostatic photovaporization, laser prostatic enucleation -HoLEP, ThuLEP-) and open surgery. It is performed under general or spinal anesthesia. They are absolutely indicated in patients who have had recurrent urinary retention, repeated urinary tract infections, upper urinary tract obstructive uropathy, and severe hematuria. These procedures try to remove all adenomatous prostate tissue, that is, the one that obstructs the urethra. Therefore, the prostate is not completely removed. All these surgical techniques are very safe and effective in expert hands such as those of our Urologists specialists of Uros but in a minority of patients complications may appear, such as infection and bleeding. Also, 1 to 3% of men develop urinary incontinence transitory or permanent. 5% of patients may also develop erectile dysfunction. After BPH surgery, most men ejaculate semen into the bladder instead of through the urethra (retrograde ejaculation).
Currently, open surgery and prostate TUR have given way to the most modern techniques with Laser (photovaporization and HOLEP or prostatic enucleation) that provide the same results but avoiding the problems derived from an incision in the skin (they are made through the duct) and also with better bleeding control.
At Uros Associats we have a super qualified team for the diagnosis, treatment and control of BPH. Several of our specialists have been pioneers in Spain in the development of various laser techniques for the treatment of prostate hypertrophy Our urologists will advise you the best treatment depending on your clinical characteristics as well as your preferences and the severity of the symptoms.
Pyeloureteral junction syndrome
Obstruction of the pyeloureteral junction (UPU) is the most common cause of hydronephrosis (dilation of the urinary system) in childhood. It affects 1 in 1,500 pregnancies. It occurs as a result of the narrowing of the junction between the renal pelvis and the ureter. Obstruction of the UPU causes a restriction of urinary flow from the pelvis to the proximal portion of the ureter and, as a consequence, there is a retrograde increase in pressure in the renal pelvis. This increase in pressure causes damage to the functional mass of the kidney, and can lead to functional annulment of the kidney.
The diagnosis of this pathology has varied greatly in recent years, being detected in early stages, even before birth. This is due to the performance of follow-up ultrasounds in all pregnant women.
It is more common in men than in women with a 3-4/1 ratio, affects more frequently the left kidney (up to 60%) and in 20-40% of cases occurs in both kidneys.
Symptoms
Before the use of prenatal ultrasound, the most common forms of presentation were abdominal pain sometimes accompanied by vomiting, urinary tract infection and haematuria macroscopic spontaneous or after a banal trauma. Other symptoms were abdominal mass and diffuse gastrointestinal discomfort. Although more rare, in some cases obstructive hydronephrosis was a casual ultrasound finding. Despite prenatal diagnosis, children are still diagnosed with symptomatic hydronephrosis at later ages. In these cases, the delay in diagnosis can lead to severe damage to the renal parenchyma, which is sometimes irreversible. However, patients diagnosed in late childhood, even in adulthood, are described in whom kidney function is preserved.
Aetiology
Congenital stenosis of UPU is generally secondary to congenital malformations that determine alterations in the amount and orientation of the ureteral muscle layers and prevent the conduction of the peristaltic wave of the excretory system.
Obstruction of late UPU is usually secondary to extrinsic compression of the ureter. The most frequent cause is the existence of Aberrant polar vessels. These aberrant vessels are usually branches of the renal artery or even the aorta, variants of renal vascular anatomy and normally supplying the lower pole of the kidney. Less commonly, compression is caused by angulations of the ureter, retroperitoneal fibrosis, or flanges caused in previous surgeries. In these cases, hydronephrosis is not present at birth and the accumulation of a certain amount of urine in the renal pelvis is necessary to stop the flow of urine, so that the increase in pressure only manifests intermittently.
Diagnosis
The primary diagnosis is usually made by ultrasound. Casual, because many congenital cases are totally asymptomatic. It will then be completed with functional tests, such as the CT-urography or intravenous urography, and, above all, the diuretic renogram. The renogram allows to assess the degree of obstruction before a dilation of the urinary tract, also providing information on the function of each kidney separately.
Treatment
Many cases of UPU syndrome require no more than close follow-up, with periodic functional imaging tests and kidney function tests.. These are asymptomatic cases and those in which the renogram does not demonstrate a significant alteration of the excretory function of the affected kidney.
In the presence of significant obstruction or the association of clinical infection or abdominal pain, it will be solved by surgery.. The most used technique is the “pyeloplasty”, consisting of the removal of the affected pyeloureteral junction and the anastomosis (union) of the pelvis to the ureter, usually leaving a catheter that will be removed in the postoperative period. It can be performed by open, laparoscopic or robotic surgery, depending on the age of the patient and availability of the center, with very similar results (good results in more than 90% of cases).
Other options that can be used are balloon dilations or cutting inside the pyeloureteral junction endoscopically (electric / laser). Its results are good, although somewhat lower than in pyeloplasty, being more recommended in cases of restenosis.
Ureteral stricture
The ureters are the tubes that carry urine from the kidneys to the bladder. In the ureter, scar tissue can form after an accident or surgery. It can also form due to a health problem, such as endometriosis or cancer. That scar tissue causes the ureter to narrow. This condition is known as stenosis. Urine cannot pass through the ureter properly and collects in the kidney, which can be painful. It can also cause urinary tract and kidney infection or kidney damage.
Aetiology
The different processes that can cause the formation of ureteral stenosis are generally associated with decreased blood flow of the affected ureter, trauma in previous interventions, periurethral fibrosis or neoplasms. The radiotherapy Applied to the pelvis or abdomen, used to treat tumors of other organs, it can be one of its causes.
Ureteral stricture can be caused by benign processes such as: Lithiasis, fibrosis (aortic aneurysm, endometriosis), infections (tuberculosis, schistosomiasis), iatrogenic lesions (open surgery, endoscopic instrumentation) or benign neoformations of the ureter. There are malignant processes capable of causing ureteral stenosis: Malignant neoformations of the ureteral wall, metastatic tumors of the cervix, ovary, colon-rectum, prostateetc.
Symptoms
The most common symptom of ureteral stricture is renal colic, almost identical to that experienced when you have a stone inside the ureter.
In addition, it is common for patients with this type of pathology to have more urinary tract infections of the upper tract (pyelonephritis).
Kidney failure It is a consequence of severe and evolved stenosis, since chronic obstruction to the physiological excretion of urine from the affected kidney causes it to be canceled. If the other kidney cannot meet the body’s fluid and electrolyte filtration needs, kidney failure will set in.
Diagnosis
Medical history (history of previous urinary instrumentation, nephritic colic, pelvic or abdominal surgery, radiotherapy, tumors, etc.) It is essential to suspect ureteral stenosis. In addition, various complementary resources are used:
- Imaging tests. Such as ultrasound, tomography, intravenous urography, retrograde or anterograde pyelography, and renal scan.
- Blood and urine tests. They allow to detect renal failure and associated infections.
Treatment
Treatment is multimodal, and almost always requires some minimally invasive or invasive intervention.
Urinary diversion. It is usually the first therapeutic act. A JJ catheter or nephrostomy catheter is placed, whose function will be to recover and / or maintain the function of that renal unit. In addition, in case of upper tract infections, such as obstructive pyelonephritis or urinary sepsis, it is a very effective emergency therapy.
Endoscopic treatment.
- Ureteral dilatation balloons, the therapeutic success of which approaches 60% in stenosis of 1 cm or less. There are several types: cutting, diathermic and barometer-controlled.
- Placement of ureteral stents, more effective in stenoses of malignant origin (cancers), with successes approaching 80% one year after placement. They can migrate in 3% of cases, and produce perforations of the ureter in 1%.
- Placement of metal ureteral catheters. They are effective in 60% of non-malignant stenosis, with a lower success rate in malignant and radiotherapy-induced stenosis.
- Endoscopic ureterotomy with Holmium laser. It has a success of 60% at 2 years of follow-up. The complication rate is low, at around 5%.
Surgery
Ureteroplasty is a surgery performed to solve the stricture.
Surgery can be performed laparoscopically, robotic surgery, or it can be done through open surgery.
Ureteroplasty can be performed by ureteral reimplantation, bladder mucosal flaps, buccal mucosal grafts or through interposition of vascularized segments of small intestine. These techniques will be chosen depending on the extent and location of the stenosis.
Urethral stricture
Urethral stenosis is a scar that narrows some point of the urethral canal, restricting the flow of urine from the bladder to the outside. It can cause a variety of urological problems, including infection or urinary retention.
Symptomatology
Signs and symptoms of urethral stricture include:
- Decreased urine flow
- Incomplete emptying of the bladder
- Urine drop by drop
- Difficulty, straining, or pain when urinating
- Increased need to urinate or more frequent urination
- Urinary tract infection
Aetiology
Scarring that can shrink the urethra may be due to:
- Iatrogenic after medical instrumentation, from probing to transurethral surgery.
- Intermittent or long-term use of a tube inserted through the urethra to drain the bladder (catheter).
- Trauma or injury to the urethra or pelvis.
- An enlarged prostate or previous surgery to remove or shrink an enlarged prostate gland.
- Cancer of the urethra or prostate.
- Sexually transmitted infections.
- Radiotherapy.
Urethral tightness is more common in men than in women. The cause is often unknown.
Diagnosis
Clinical questioning is mandatory. It asks about urinary symptoms and how they affect the patient’s quality of life. In addition, their surgical history or urinary instrumentation, sexually transmitted infections, etc. are investigated.
The complementary tests requested are:
- Urinalysis: looks for signs of infection, blood, or cancer in the urine
- Flowmetry: measures the strength and amount of urine flow
- Pelvic ultrasound: looks for urine in the bladder after you urinate
- Retrograde urethrography: uses x-rays to look for a structural problem or injury to the urethra, as well as analyze the extent and location of urethral stricture
- Cystoscopy: examines the urethra and bladder with a thin, tube-like device that has a lens (cystoscope) to look at these organs
Treatment
The treatment will depend on each case. Available treatment options include:
- Catheterization. The most common first step in treating urine obstruction is to insert a small tube (catheter) into the bladder to drain it.
- Dilatation. The doctor inserts a small cannula through the urethra that goes into the bladder. Larger and larger dilators are passed over the cannula to gradually increase the size of the urethral opening. This outpatient procedure may be an option for recurrent urethral strictures.
- Urethroplasty. It is a procedure that involves the surgical removal of the narrowed parts of the urethra or widening of the urethra. In addition, the procedure could involve reconstruction of surrounding tissues. In short strictures it is possible to dry out the damaged part of the urethra and join the ends with stitches (end-of-end urethroplasty). In longer stenosis, tissues from other areas of the body, such as the skin or buccal mucosa, can be used to make grafts during reconstruction (urethroplasty with graft).
- Endoscopic urethrotomy. For this procedure, your doctor inserts a thin optical device (cystoscope) into your urethra, then inserts instruments through the cystoscope to section the stenosis or vaporize it with a laser. This surgical procedure has a faster recovery, leaves minimal scarring, and presents less risk of infection, although there is a chance of recurrence.
- Implanted stent or indwelling catheter. In certain cases, an artificial permanent tube (stent) may be chosen to keep the urethra open or an indwelling catheter to drain the bladder. However, these procedures have several disadvantages, such as the risk of bladder irritation, discomfort, and urinary tract infections. In addition, they need to be closely monitored. Generally, urethral stents are a measure of last resort and are not usually used.
Laser in Urology
Laser means “Light Amplification by Stimulated Emission of Radiation”.
It is a technology increasingly used in minimally invasive endourological procedures, improving the therapeutic arsenal of the urologist in a large number of pathologies.
The LASER system has certain advantages over other tissue cutting systems, such as: the transmission of large amounts of energy through flexible fibers, high safety and efficiency, due to the low risk of injury to adjacent structures, selectivity by specific tissues according to wavelength and a wide margin of action, due to the ability to regulate both the amount of energy emission transmitted, as well as its frequency.
There are different types of lasers depending on their wavelength, frequency and tissue penetration. The most used in urology are the Holmium laser, the Tulio laser and the Green laser.
Holmium Laser
It is a laser with a wavelength of 2,140 nm and a minimum penetrability in the tissue of 0.4 mm and is absorbed by water. It allows the realization of different minimally invasive techniques. This makes it currently the most versatile and important type of laser in Urology.
- Benign prostatic hyperplasia. Thanks to a photothermal contact mechanism allows the enucleation of the prostate (prostatic enucleation with Holmium laser), avoiding the classic adenomectomy (open surgery). It allows a significant reduction in hospital stay, blood loss and urinary catheter time.
- Ureteral/urethral stenosis. It is useful in the surgery of the narrowing of the ureter, pyeloureteral junction and urethra. This laser allows to section the fibrous callus and expand the lumen of the treated duct. A catheter is left to tutor the duct for a few days or weeks.
- Urinary lithiasis. It allows to eliminate kidney stones and ureter, vaporizing or fragmenting them. The Holmium laser is used as an adjuvant in ureteroscopy, percutaneous renal surgery and endoscopic cystolithopathy. Holmium is applied at different frequencies, depending on the type of effect we want to apply on urinary calculus. If you want to vaporize or fragment into millimeter pieces we will use high frequency at low energy. If we intend to fragment into larger pieces we will use low frequency and high energy.
- Treatment of tumors of the urinary tract. Bladder and upper urinary tract tumors can be treated by vaporization. It is mainly indicated in superficial and small tumors.
Green Laser (Greenlight XPS 180 W)
It is a laser with a wavelength of 532 nm and a penetrability of 0.8 mm. It is minimally absorbed by water and much more by hemoglobin. Its fundamental application is the minimally invasive treatment of Benign prostatic hyperplasia. The technique of treatment of this condition can be fundamentally of two types.
- Prostatic vaporization. Indicated mainly in prostate of small and medium size, below 40cc. It consists of vaporizing the tissue until leaving a good channel for urination. Advantages: minimal bleeding, very short hospital stay and need for 24-hour bladder catheterization. The results are similar to those of prostate resection, but with better recovery. Mixed techniques of anatomical vaporization and vapo-enucleation can be done.
- Prostatic enucleation. Indicated in moderate and large prostates. It consists of the endoscopic reproduction of the classic open adenomectomy. It allows the complete enucleation of the adenoma and its subsequent morcellation within the bladder. Similar to adenomectomy, with comparable results, but with countless advantages. Reduces hospital stay and bladder catheterization, postoperative pain and bleeding. Also, recovery and return to normal activity is much earlier than with open surgery. This technique can also be performed with the Holmium laser, which has gradually displaced the green laser due to its great versatility, and is currently the technique of choice for prostate enucleation.
Tulio Laser
It has a variable wavelength between 1.75 and 2.22 μm, and is mainly applied in prostate hyperplasia. The techniques are similar to green laser and Holmium and in recent times it is also applied for the treatment of lithiasis. Its use is much less widespread than that of the previous lasers commented.
In Uros Associats we use laser technology in all endourological procedures in which it can be used, since we understand that it represents the ideal system for the minimally invasive and effective treatment of a wide variety of pathologies. We select each type of laser according to the characteristics of each patient and each pathology, since we can have all of them. We have expert specialists in the application of laser technology in urology, both in the treatment of lithiasis, enucleation and prostatic vaporization, and in the conservative management of urinary tract tumors.
- PROSTATIC ENUCLEATION WITH HOLMIUM LASER.
- TRANSURETHRAL RESECTION OF THE PROSTATE.
- PROSTATIC PHOTOVAPORIZATION.
- HOLEP.
- INTERNAL OR ENDOSCOPIC URETHROTOMY.
- TERM-TERMINAL URETHROPLASTY.
- URETHROPLASTY WITH ORAL MUCOSA.
- LAPAROSCOPIC PEELOPLASTY.
- ROBOTIC PEELOPLASTY.
- LAPAROSCOPIC URETERAL REIMPLANTATION.
- ROBOTIC URETERAL REIMPLANTATION.
The prostate is a gland of the male reproductive system that, together with the seminal vesicles, is responsible for producing semen. It is the size of a walnut and is located under the bladder, in front of the rectum. But over the years, its central part can grow to the point of compressing the urethra, causing what is known as the benign prostatic adenoma.
This obstruction can cause difficulty emptying the bladder, a phenomenon that affects more than half of men over 50, half of whom require treatment.